Circulatory System
The circulatory system delivers oxygen (O2) and nutrients to the cells of the body and transports carbon dioxide (CO2) to the lungs and metabolic wastes to the kidneys.
Table of Contents
- Animal Circulatory System: An Overview
- The Human Cardiovascular System
- Download Article in PDF Format.
- Test Yourself!
Animal Circulatory System: An Overview
To sustain life, animals must acquire nutrients, exchange gases, and dispose of waste products. These processes are facilitated by the circulatory system.
A circulatory system is necessary for animals with large bodies or too complex a structure for diffusion to occur alone. This internal transport system must bring resources closer to cells for diffusion to be effective. Animals with multiple layers of cells require a true circulatory system. This kind of internal transport consists of a muscular pump called a heart, a circulatory fluid, and a set of tubes/vessels to carry the fluid.
Two basic types of the circulatory system evolved in animals: an open circulatory system is apparent in many invertebrates, such as mollusks and arthropods; and a closed circulatory system such as that of our own. An open circulatory system is considered open because the circulatory fluid is not distinct from the interstitial fluid, the fluid that fills the spaces between cells. In a closed circulatory system, the circulatory fluid “blood” is confined to blood vessels being distinct from the interstitial fluid.
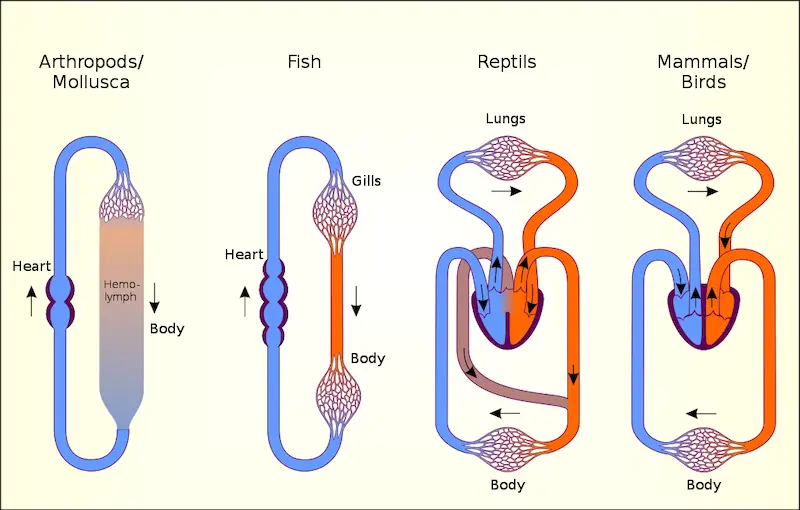
Three kinds of blood vessels are present in our body: arteries carry blood away from the heart and towards the body organs and tissues; veins return blood to the heart, and capillaries convey blood between the arteries and veins within each tissue. The vertebrate circulatory system is often called a cardiovascular system because of the heart and extensive blood vessels that when lined end to end, would be able to circle Earth’s equator twice.
The circulatory system of a fish illustrates some key features of a closed circulatory system. Two main heart chambers: the atrium, which receives blood from the veins, and the ventricle which pumps blood to the gills via large arteries. Large arteries branch into arterioles which give rise to capillaries. Networks of capillaries called capillary beds infiltrate every organ and tissue in the body. The capillaries converge into venules, which in turn converge into larger veins that return blood to the heart. This arrangement is called a single circulation since blood passes through the heart only once and when animals began to colonize land, a need for the system to adapt to land ensued.
A single circuit is not enough to move blood to the capillaries of the lungs and then to the capillaries in the body of land animals so an adaptation led to what is called a double circulation, in which blood is pumped a second time after it loses pressure in the lungs. Two circuits compose this with the pulmonary circuit carrying blood between the heart and gas exchange tissues of the lungs, and the systemic circuit which carries blood between the heart and the rest of the body.
Frogs and other amphibians have a three-chambered heart. The right atrium receives blood returning from the systemic capillaries in the body’s organs. The ventricle pumps blood to capillary beds in the lungs and skin. Because these animals can exchange gases in their moist skin, this is called a pulmocutaneous circuit. The oxygen-rich blood returns to the left atrium. Although blood from the two atria mixes in a single ventricle, a ridge diverts the oxygen-poor blood to the pulmocutaneous circuit and the oxygen-rich blood to the systemic circuit.
In the three-chambered hearts of turtles, snakes, and lizards, the ventricle is partially divided, and less mixing of blood occurs. The ventricle is completely divided in crocodilians. In birds and mammals, the heart has four chambers: two atria and two ventricles. The right side of the heart handles only oxygen-poor blood and the left side receives and pumps only oxygen-rich blood.
We will now take a closer look at the human cardiovascular system, starting with the mechanisms of the heart.
The Human Cardiovascular System
In the pulmonary circuit, the pulmonary arteries carry oxygen-poor blood to the lungs. Blood flows back into the heart through the pulmonary veins, which bring oxygen-rich blood from the lungs. In the systemic circuit, oxygen-rich blood exits the heart via the aorta. After journeying through the body, the superior vena cava returns oxygen-poor blood to the heart from the upper body while the inferior vena cava returns oxygen-poor blood from the lower body.
1. The Heart
The heart is about the size of a clenched fist and is formed mostly of cardiac muscle tissue. The ventricles, which pump blood to the lungs and body, have much thicker walls than the atria. The thin-walled atria collect blood returning to the heart and squeeze it into the ventricles below.
What keeps blood flowing in one direction is the presence of flap-like valves made of connective tissue which are found in the exit from each chamber. The valves between the atria and ventricles are called atrioventricular (AV) valves while those found at the exit of each ventricle are the semilunar valves. These valves open when pushed from one side and close when pushed from the other, preventing backflow.
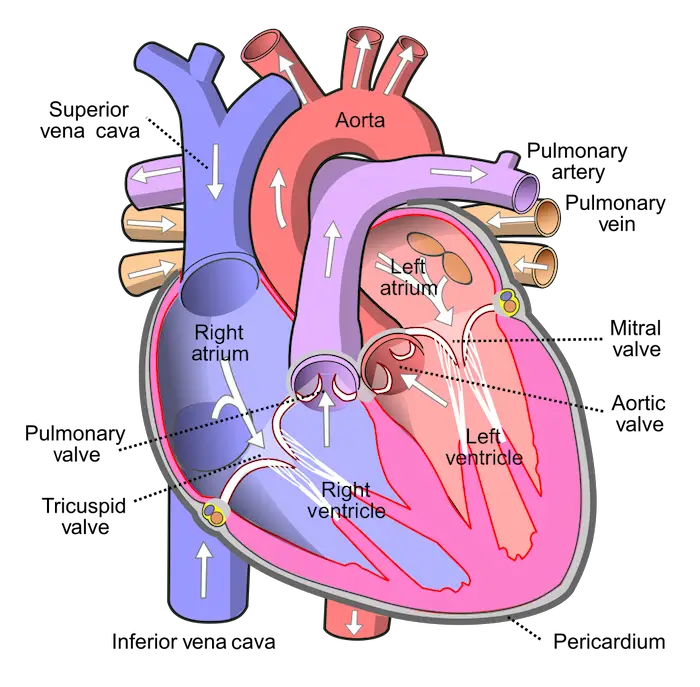
By the way, if you look at images or illustrations of most organs (e.g., the illustration of the heart above), most are oriented as if you are facing another person, so you might have observed that parts which are labeled “left” are seen on your right, and vice versa.
You can hear the closing of the heart valves with a stethoscope or by pressing your ears against the chest, with a sound pattern being “lub-dub, lub-dub, lub-dub…” with the “lub” sound coming from the recoil of blood against the closed AV valves while the “dub” is blood against the semilunar valves. When a valve is defective, blood may squirt backward and may produce an abnormal sound called a heart murmur.
The Cardiac Cycle
The heart contracts and relaxes in a normal rhythmic sequence known as the cardiac cycle. When the heart contracts, it pumps blood and when it relaxes, blood fills its chambers. In a phase called diastole, the heart relaxes and blood flows into all four chambers. Blood enters the right atrium from the vena cava and the left atrium from the pulmonary veins. The AV valves are open while the semilunar valves are closed. The ventricles nearly fill with blood during diastole.
The contraction phase of the cycle is called systole. It begins with a brief contraction of the atria that completely fill the ventricles with blood (atrial systole). The ventricles then contract (ventricular systole) and the force closes the AV valves but opens the semilunar valves, where the blood is pumped into large arteries. Blood flows into the relaxed atria during the second part of the systole.
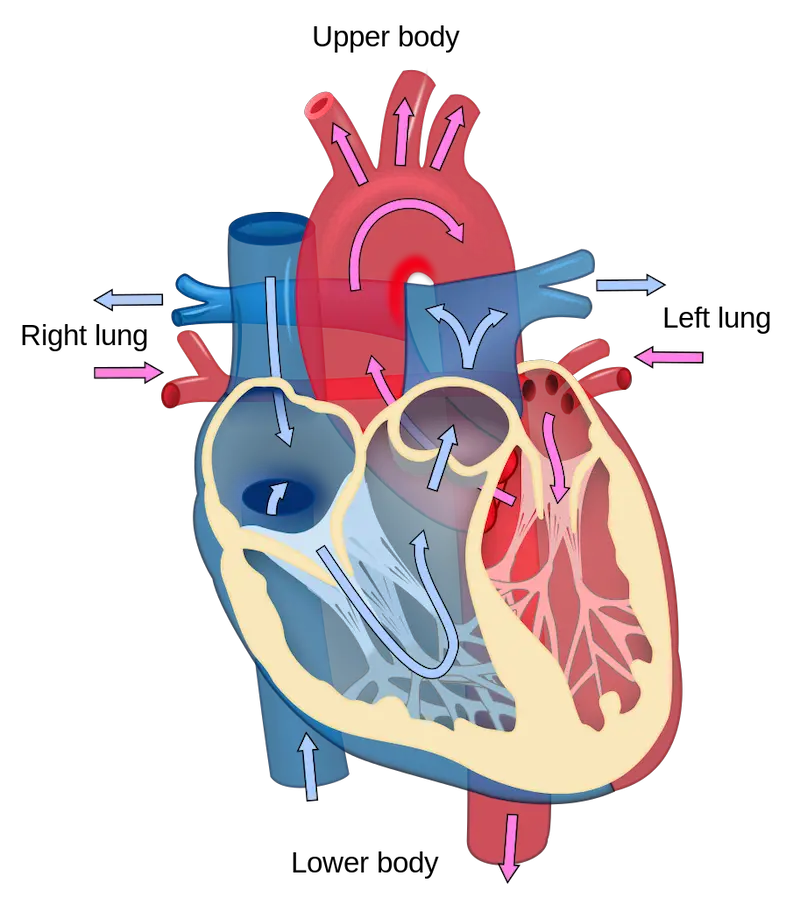
The left ventricle contracts with greater force than the right because it pumps blood to the whole body thus having a thicker wall. Both ventricles, however, pump the same volume of blood. The volume of the blood that each ventricle pumps per minute is called the cardiac output. This volume is equal to the amount of blood pumped each time a ventricle contracts times the heart rate or the number of heartbeats per minute.
The contraction and relaxation of each chamber of the heart must follow a precise sequence and timing to pump blood through the body. How does the contraction of cardiac cells coordinate heartbeats so well? The answer lies with a group of cells that make up the SA (sinoatrial) node, or pacemaker, which sets the rate at which all the muscle cells of the heart contract.
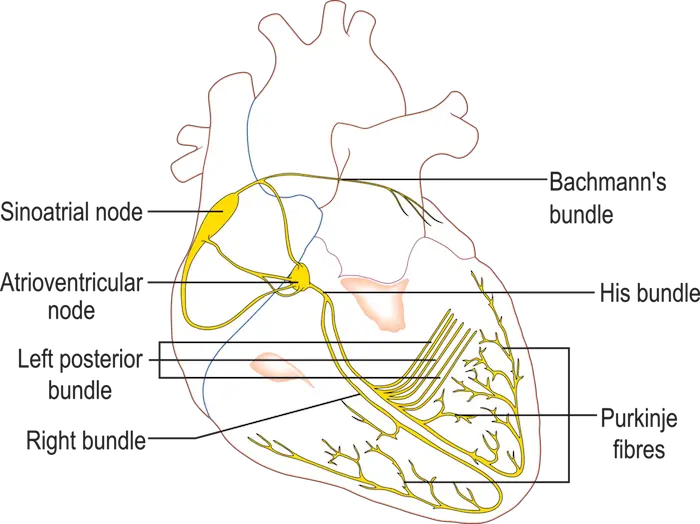
The SA node, situated in the upper wall of the right atrium generates electrical impulses that spread rapidly through specialized junctions between cardiac muscle cells called the intercalated disks.
Signals from the SA node spread quickly through both atria, making them contract in unison. The impulses pass to the AV (atrioventricular) node, between the right atrium and right ventricle. The AV node delays the signal, enough for the atria to empty, before the ventricles contract. Specialized muscle fibers then relay signals to the apex of the heart and up through the walls of the ventricles, triggering the strong contractions that drive the blood out of the heart.
These impulses are strong enough to be detected on the skin by electrodes and recorded as an electrocardiogram (ECG) which can provide data about heart health such as the existence of arrhythmias, abnormal heart rhythms.
Like all other tissues, heart muscle cells require nutrients and oxygen-rich blood to survive. Coronary arteries supply these and in cases where one or more of the blood vessels become completely blocked, heart muscle cells quickly die leading to a heart attack or myocardial infarction. The ability of the heart to pump blood after this event may be seriously impaired.
Other diseases that may arise include stroke which is the death of brain tissue due to lack of oxygen brought about by the rupture or blockage of arteries supplying blood to the brain. Another is atherosclerosis, a chronic cardiovascular disease wherein fatty deposits called plaques develop in the inner walls of arteries, narrowing passages through which blood can flow.
The heart is just one component of the cardiovascular system. Blood vessels, on the other hand, form a web-like structure in our body and will be our focus next.
2. The Blood Vessels
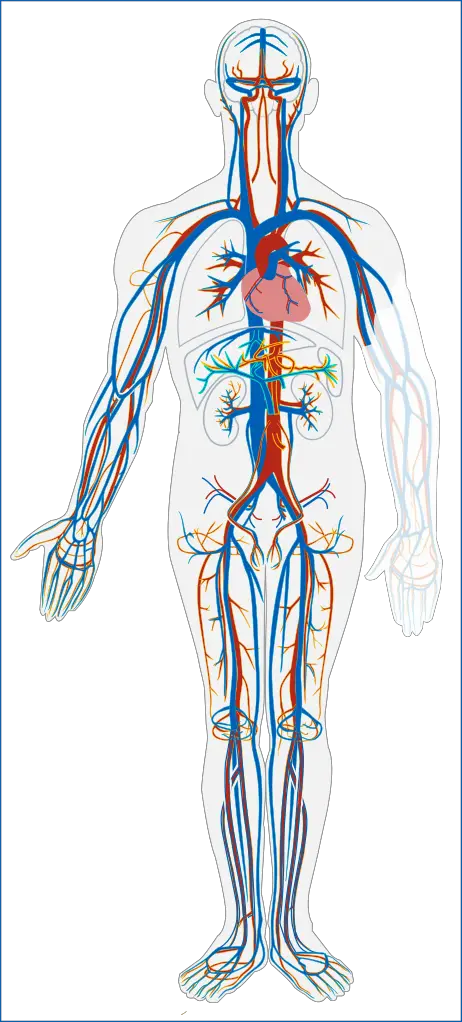
All blood vessels are lined by epithelium with the different sizes and structures of the blood vessel reflecting the roles they play in transporting materials and exchanging them with tissues in the body. Blood vessels are classified into three:
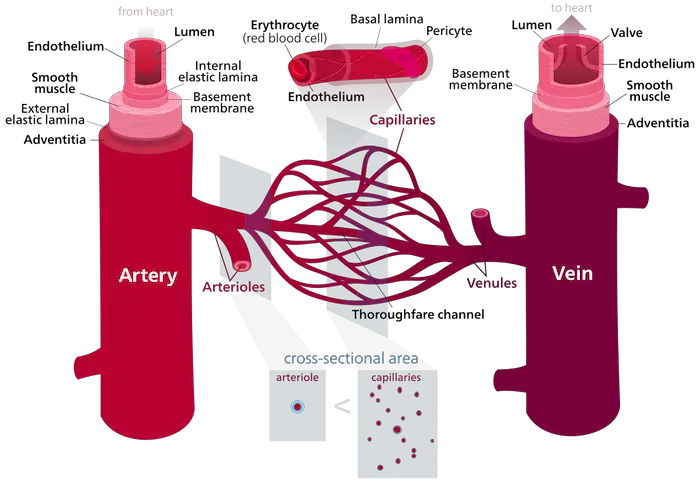
“Blood vessels” by Kelvinsong is licensed under CC BY-SA 3.0.
a. Arteries
Their key function is to transport blood from the heart to the lungs and other parts of the body. Arteries have the thickest walls amongst blood vessels, providing strength and elasticity to accommodate the rapid flow and high pressure of blood pumped by the heart.
An outer layer of connective tissue with elastic fibers enables the vessels to stretch and recoil. Smooth muscles in the walls of arteries and arterioles narrow or widen the vessels in response to hormones and signals from the nervous system. The constriction or relaxation of the vessels modulates blood flow to different parts of the body.
b. Capillaries
Unlike other blood vessels, capillaries consist of only a single layer of epithelial cells wrapped in an extracellular matrix. This structure fits their unique function: exchange. Facilitating this exchange is their close connection with the tissues in the body. In addition to providing oxygen and nutrients to cells, capillaries also pick up metabolic wastes.
c. Veins
As blood exits capillaries in the tissues, it enters venules and then veins. These vessels transport blood from the lungs and other parts of the body to the heart. Velocity and pressure are lower in veins than in arteries and it is reflected in that the walls of veins are thinner than those of arteries. Large veins have flaps of tissue that act as one-way valves, permitting blood to flow only toward the heart.
The forces that move blood through these vessels include:
- Blood pressure – the force blood exerts on the walls of blood vessels. Created by the pumping of the heart, blood pressure drives the flow of blood from the heart through arteries and arterioles to capillary beds. When the ventricles contract, blood is forced into the arteries faster than it can flow into arterioles. This rhythmic stretching of the arteries can be felt when measuring heart rates with our pulse. Blood pressure in the arteries depends on the volume of the blood pumped into the aorta and the restriction of blood flow into the narrow openings of the arterioles.
- Blood velocity – refers to the rate of flow (measured in cm/sec). Velocity declines rapidly in the arterioles, drops to zero in capillaries, then speeds up in veins.
The heart, the blood vessels, what else is there? Oh! The blood. We will now look closer at the blood, like vampires homing into its prey *looks nervously at Dinuguan as if it isn’t a part of Philippine cuisine*.
3. The Blood
Blood consists of several cells suspended in a liquid called plasma. When a blood sample is taken, the cells can be separated from the plasma by spinning in a centrifuge. The cellular components making up about 45% of the volume of the blood settle to the bottom of the centrifuge tube, while the transparent, straw-colored plasma rises.
Plasma is about 90% water and is also made of inorganic salts in the form of dissolved ions (electrolytes) that function in keeping the blood’s pH stable and maintaining the osmotic balance between blood and interstitial fluid.
Plasma proteins, such as albumin, act as buffers that help maintain osmotic balance. Fibrinogen is a plasma protein that functions in blood clotting, and immunoglobulins are important in immunity. Apolipoproteins escort insoluble lipids, which can travel blood only when bound to proteins.
There are two classes of cells suspended in the plasma: white blood cells and red blood cells. Platelets are also suspended and these are cell fragments involved in the process of blood clotting. There are five major types of white blood cells (WBCs) or leukocytes with their collective function in fighting infections: monocytes, neutrophils, basophils, eosinophils, and lymphocytes.
For example, monocytes and neutrophils are phagocytes that engulf and digest bacteria; basophils release histamine which is used in the inflammatory response; eosinophils attack parasites and cancer cells while helping in the allergic response, and lymphocytes have other functions related to immunity.
Red blood cells (RBCs) are also called erythrocytes and their main function is to carry oxygen. RBCs are small biconcave disks, thinner in the center than at the sides which allow for a large surface area for oxygen to diffuse into. When an RBC matures, it lacks a nucleus, allowing more room to pack in hemoglobin, which gives the blood its red color.
The Blood Clotting Process
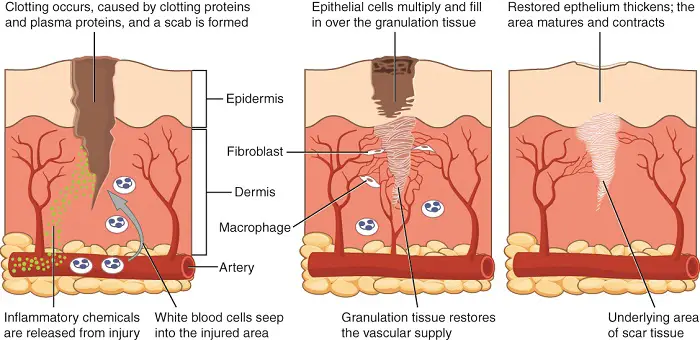
As mentioned earlier, fibrinogen is a protein needed in blood clotting. When we sustain an injury, the body’s immediate response is to constrict the damaged blood vessel to reduce blood loss and allow time for repairs to begin.
When the epithelium lining a blood vessel is damaged, the connective tissue in the vessel wall is exposed to blood. Platelets rapidly adhere to the exposed tissue and release chemicals that make nearby platelets sticky. Soon the cluster of sticky platelets forms a plug that provides protection against additional blood loss.
Clotting factors in the plasma and released from the platelets set off a chain reaction that ultimately forms a reinforced patch that keeps blood from leaking into the surrounding tissue. Think of it as a scab inside a vessel.
In this complex process, an activated enzyme converts fibrinogen into a threadlike protein called fibrin. Threads of fibrin reinforce the plug, forming a clot. The clotting mechanism is so important that any defect in it can be life-threatening.
Hemophilia is a condition leading to excessive and sometimes fatal bleeding that is attributed to either one or more proteins required for clotting being absent in individuals with the condition. In other people, blood clots may form in the absence of injury. Such a clot called a thrombus can be dangerous if it blocks blood going to the brain or heart.
For healthy body functions, adequate numbers of RBCs are essential. An abnormally low amount of hemoglobin or red blood cells is a condition called anemia. The production of red blood cells in the bone marrow is controlled by a negative feedback mechanism that is sensitive to the amount of oxygen reaching the tissues via the blood. If the tissues are not getting enough oxygen, the kidneys produce erythropoietin (EPO), a hormone that stimulates RBC production in the bone marrow.
Leukemia is the cancer of white blood cells. Because cancer cells grow uncontrollably, a person with leukemia has an unusually high number of WBCs, most of which are defective. These overabundant cells crowd out the bone marrow cells that are developing into red blood cells, and platelets, causing severe anemia and impaired clotting.
The body has developed means to maintain and get rid of cells that go haywire to prevent itself from being jeopardized. Next, we will take a closer look at the organs and mechanisms involved in maintaining our immunity.
Next topic: Immune System
Previous topic: Respiratory System
Return to the main article: Animal Form and Functions (Overview)
Download Article in PDF Format.
Test Yourself!
1. Practice Questions [PDF Download]
2. Answer Key [PDF Download]
Copyright Notice
All materials contained on this site are protected by the Republic of the Philippines copyright law and may not be reproduced, distributed, transmitted, displayed, published, or broadcast without the prior written permission of filipiknow.net or in the case of third party materials, the owner of that content. You may not alter or remove any trademark, copyright, or other notice from copies of the content. Be warned that we have already reported and helped terminate several websites and YouTube channels for blatantly stealing our content. If you wish to use filipiknow.net content for commercial purposes, such as for content syndication, etc., please contact us at legal(at)filipiknow(dot)net